
Disclaimer: The information provided on bunnyowners.com is for educational purposes only and does not constitute veterinary medical advice; always consult your vet before changing your rabbit’s diet. Additionally, this post contains affiliate links. As an Amazon Associate, and other affiliate advertising programs, I earn from qualifying purchases at no extra cost to you
Rabbit head tilt, or wry neck, is a sudden sideways rotation of the neck caused by vestibular dysfunction. While symptoms like circling or rolling are distressing, it is vital to remember that head tilt is a clinical sign of an underlying issue, not the disease itself. Recognizing these early SOS signals is the first step toward effective treatment and recovery. What causes head tilt in rabbits?
Rabbit head tilt (wry neck) is primarily caused by inner ear infections (Otitis interna), the parasite Encephalitozoon cuniculi, vestibular system inflammation, trauma, or neurological diseases. Symptoms include a persistent sideways tilt, uncontrollable rolling, loss of coordination, and rapid involuntary eye movements (nystagmus). Because head tilt can lead to life-threatening GI stasis and severe dehydration, it is classified as a veterinary emergency requiring immediate medical intervention.
Fortunately, head tilt is not an automatic death sentence; early stabilization and aggressive nursing care lead to high recovery rates. Whether a rabbit regains full balance or adapts to a permanent “perky” tilt, they can still lead a happy life when managed under proper rabbit health protocols. This guide breaks down the causes, the diagnostic “shotgun” approach used by specialists, and the comprehensive care required to help a “wonky” bunny recover.
2. Defining Head Tilt and Vestibular Disease
Definition of the Condition
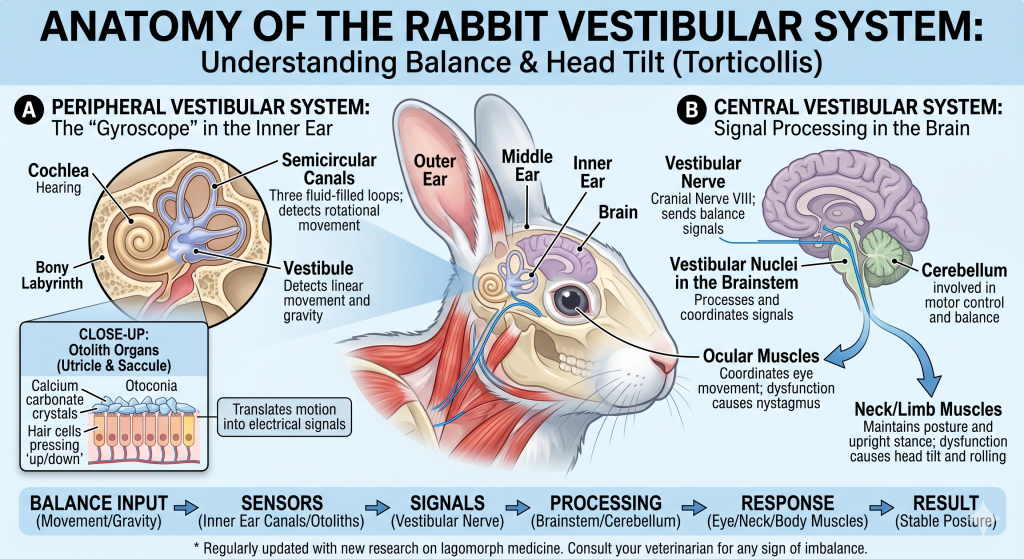
Technically known as vestibular disease or torticollis, head tilt occurs when the rabbit’s balance system—comprised of the inner ear and the brainstem—suffers a communication breakdown. The vestibular system is responsible for telling the rabbit which way is “up” and ensuring their ocular muscles coordinate with their movement to maintain a stable visual field. When this system is compromised, the brain receives scrambled data, making the rabbit feel as though the floor is permanently shifting, tilting, or vanishing entirely.
In rabbits, the vestibular apparatus is highly sensitive. The peripheral portion resides in the inner ear (the semicircular canals and the vestibule), while the central portion involves the vestibular nuclei in the brainstem and the cerebellum. Inflammation or damage at any point along this pathway results in the characteristic “lean.” Unlike humans, who might simply feel dizzy, a rabbit’s instinct is to physically rotate their entire body to match the perceived tilt, leading to the dramatic neck twist we see.
Mechanisms of Balance Loss
The vestibular system controls orientation through fluid-filled canals in the ear and neural pathways in the brain. If inflammation, infection, or a parasite disrupts these signals, the “ear-to-brain” loop breaks. The rabbit physically twists its neck to match what it thinks is the horizontal plane. This disruption can be so profound that the rabbit loses the “righting reflex”—the natural ability to stay on their paws.
When a rabbit feels they are falling, they often panic. This panic triggers a cycle of thrashing and rolling. This isn’t a seizure; it is a desperate attempt to find “up.” In some cases, the rabbit will roll so violently that they can cause spinal fractures or severe eye ulcerations from rubbing against the floor. Understanding that this is a mechanical failure of the balance sensors—not a lack of will—is crucial for owners providing supportive care. To see how these mechanics fit into a broader clinical recovery plan, refer to my rabbit health guide.
Terminology and Classifications
- Head Tilt: The layperson’s term for the visual symptom.
- Wry Neck: An older, descriptive term often used in agricultural contexts.
- Peripheral Vestibular Disease: Issues specifically within the inner ear structures. These often have a better prognosis if the infection is caught before it enters the brain.
- Central Vestibular Disease: Issues involving the brain and central nervous system. This is frequently associated with E. cuniculi or brain abscesses and can be harder to treat.
3. Clinical Symptoms of Head Tilt

Early Warning Signs
The earliest red flags are often subtle. You might notice a slight 5-degree lean or a rabbit that is suddenly “clumsy” when hopping onto a favorite perch. Because grooming requires a fair amount of twisting and balance, a rabbit in the early stages of tilt may stop cleaning their back or ears to avoid the dizziness that comes with movement. You might also notice their ears are held at different heights, or one ear seems “heavy.”
Another early indicator is a change in jumping accuracy. If your rabbit usually clears a 12-inch barrier with ease but is now hesitating or clipping the top with their back feet, their depth perception and balance are likely beginning to falter. These mild signs are the “Golden Window” for treatment; intervention at this stage can often prevent the more traumatic symptoms from developing.
Progression of Symptoms
As the underlying cause progresses, the tilt becomes unmistakable. The rabbit will begin circling in one direction or falling sideways when trying to eat. At this stage, they may lean their body weight against the side of their enclosure for support, and reaching a water bowl becomes a physical challenge. The rabbit may also exhibit “metabolic” changes, appearing lethargic or showing a decreased interest in their favorite greens.
Circling is particularly common when the vestibular deficit is unilateral (on one side). The rabbit feels a constant pull toward the affected side and will literally walk in loops. This can be exhausting for the animal and often leads to sores on the feet (pododermatitis) from the repetitive, uneven friction. Detailed medical breakdowns of these presentations can be found at MediRabbit.
Advanced Symptoms and Eye Movements
In severe cases, rabbits experience uncontrollable rolling—spinning like a top until they hit an obstacle. This is almost always accompanied by nystagmus, which are rapid side-to-side or rotary eye movements. As the Merck Veterinary Manual explains, nystagmus indicates that the brain is frantically trying to fix a visual horizon it perceives is moving.
| Symptom Severity | Physical Manifestations | Action Level |
| Mild | Slight head angle, clumsy hopping, reduced grooming | Schedule vet visit within 24 hours |
| Moderate | Clear 45-degree tilt, circling, stumbling | Urgent vet care needed today |
| Severe | Continuous rolling, unable to stand, rapid eye flicking | Immediate Emergency |
4. Why Head Tilt is a Medical Emergency
Risk of Digestive Shutdown
Rabbits are physiologically fragile; their biggest enemy during a tilt episode is their own digestive tract. The nausea and stress often cause a rabbit to stop eating and drinking entirely. Within hours, this can trigger GI stasis, where the gut stops moving. Once the gut shuts down, gas builds up, causing extreme pain, which further decreases the rabbit’s willingness to eat, creating a lethal cycle.
Because rabbits have a high metabolic rate, they cannot go for long periods without calorie intake. In a head tilt rabbit, the “seasickness” they feel makes the smell and texture of food unappealing. If you see the rabbit “chinning” their food but not eating it, or if their fecal pellets are becoming smaller and drier, stasis is already setting in.
Physical Injuries and Stress
Rolling rabbits are at high risk for physical trauma. They can easily scratch their eyes against cage bars, break limbs, or suffer spinal injuries. The psychological stress of being unable to stand can send a prey animal into shock. A rabbit in shock will have pale mucous membranes, cold ears, and a rapid, shallow heart rate.
To a rabbit, the inability to run represents a complete loss of their primary defense mechanism. This “helplessness” leads to a massive release of cortisol, which can suppress the immune system right when they need it most to fight off an ear infection or parasite. This is why supportive care—keeping them calm and physically secure—is just as important as the medication itself.
5. Primary Causes of Head Tilt
Bacterial Ear Infections
This is the most common culprit. Bacteria (like Pasteurella multocida) migrate from the nasal cavity through the Eustachian tube into the inner ear. Curiously, a rabbit can have a massive inner ear infection without any visible discharge in the outer ear, making it a “hidden” illness. The infection produces pus (which in rabbits is thick and cheese-like), putting pressure on the delicate vestibular nerves.
A rabbit can have a massive inner ear infection without any visible discharge in the outer ear, making it a “hidden” illness. This is why “standard” ear exams with an otoscope are often insufficient for a definitive diagnosis. Chronic ear infections are notorious for being difficult to treat because the antibiotics have a hard time penetrating the thick pus and the dense bone of the ear canal. Research on rabbit otitis shows that aggressive, long-term therapy is usually required to resolve these cases.
E. Cuniculi Parasitic Infection
This microscopic parasite targets the brain and kidneys. It is incredibly common in the rabbit population, often lying dormant until stress allows it to trigger inflammation. As the parasite replicates, it causes the rupture of host cells, leading to “granulomatous” inflammation in the central nervous system. This inflammation disrupts the neural pathways that control balance.
According to Rabbit Welfare Association & Fund (RWAF), diagnosing E. cuniculi can be difficult because a positive blood test only confirms previous exposure, not necessarily active disease. However, if kidney values are elevated or the rabbit also develops cataracts — another common sign associated with E. cuniculi — the diagnosis becomes much more likely.
6. Diagnostic Procedures for Rabbits

Physical Exams and Bloodwork
Since rabbits can’t describe their vertigo, vets rely on physical clues. They check for ear pain, evaluate the type of nystagmus, and look for “facial nerve paralysis” (a drooping lip or ear). Facial paralysis often occurs alongside ear infections because the facial nerve runs through the same bony canal as the vestibular nerve.
Bloodwork is the next step to look for white blood cell counts (indicating infection) or E. cuniculi antibody titers. An IgG/IgM titer test can help determine if the infection is active (high IgM) or a past exposure (high IgG). High kidney enzymes (BUN and Creatinine) may also suggest that the parasite is currently damaging the renal system, providing further evidence for the E. cuniculi theory.
Diagnostic Imaging Options
Standard X-rays are a starting point but often miss fine inner-ear details. A “clean” X-ray doesn’t mean the ear is healthy; it just means the bone hasn’t started to dissolve yet. For a definitive look at the ear bone (bulla), many specialists recommend a CT or MRI to reveal hidden abscesses.
A CT scan is considered the gold standard for diagnosing middle and inner ear disease in rabbits because it allows veterinarians to see whether the ear bulla is filled with fluid, infection, or abscess material. In severe cases involving deep infection or abscesses, surgery such as a total ear canal ablation or ventral bulla osteotomy may be necessary to control the disease and improve long-term survival. Clinical discussions and imaging guidance for rabbit ear disease can be found at LafeberVet
7. Treatment Protocols and Medications
Commonly Prescribed Drugs
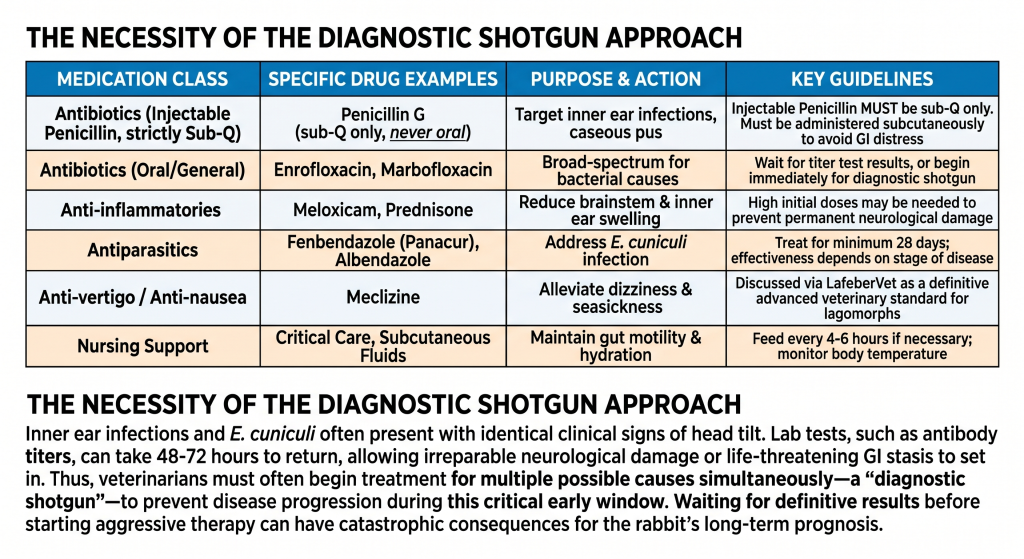
Treatment usually involves a “shotgun” approach, addressing both infection and parasites simultaneously while results are pending. Because the causes are so distinct but the symptoms are identical, waiting for a lab result can cost the rabbit their life. You can further examine the clinical efficacy of these treatment protocols to see how aggressive, early intervention directly impacts long-term survival odds.
Effective antibiotics must be able to cross the blood-brain barrier if the infection is central. Commonly used drugs include Azithromycin, Chloramphenicol, or Enrofloxacin. For E. cuniculi, the standard is a 28-day course of Fenbendazole. Without anti-inflammatories like Meloxicam, the swelling in the brain or ear can cause permanent scarring, making these drugs vital for a full recovery.
| Medication Class | Common Examples | Primary Purpose |
| Antibiotics | Enrofloxacin, Penicillin G | Eliminate bacterial ear infections |
| Antiparasitics | Fenbendazole (Panacur) | Halt E. cuniculi replication |
| Anti-inflammatories | Meloxicam (Metacam) | Reduce swelling and provide pain relief |
| Supportive Meds | Meclizine, Cisapride | Combat nausea and maintain gut motility |
8. Home Care and Nursing Support
Environment and Housing Adjustments
The “padded cell” method is your best friend. Use a small, single-level enclosure and remove all ramps. Line the floor with high-traction, soft bedding like fleece or “Vetbed” to prevent slipping. Use rolled-up towels to create “bumpers” around the perimeter to prop the rabbit up and prevent rolling. This physical support provides a sense of security that lowers the rabbit’s heart rate.
It is also important to dim the lights. Bright lights and sudden movements can overstimulate a rabbit whose visual system is already haywire. Think of it like managing a human with a severe migraine; a quiet, dark, stable environment is the foundation of healing. If the rabbit is still rolling, a very small travel carrier lined with thick padding can be used to “snug” them in and limit their movement until the medication kicks in.
Assisted Feeding and Fluid Intake
If your rabbit isn’t eating, you must intervene. Syringe feeding a recovery diet (like Critical Care) ensures the gut stays moving. You should aim for several small feedings a day rather than one large one, as a stressed rabbit’s stomach can be quite sensitive. Hydration is equally critical; a dehydrated rabbit will have thicker blood, making it harder for medications to circulate.
If a tilted rabbit cannot reach their water bowl because their head is resting against the floor, you may need to offer water carefully by syringe or switch to a shallow, heavy ceramic bowl that is easier to access. Avoid water bottles for rabbits with head tilt, since they often cannot position themselves correctly to use the spout and may become frustrated or dehydrated. For syringe-feeding and supportive care techniques, find detailed instructions on assisted feeding techniques for rabbits on Veterinary Partner.
9. Prognosis and Recovery Expectations

Stages of Improvement
Recovery is measured in weeks, not days. Patience is required as the brain rewires its balance signals. You may see “good days” followed by “bad days,” especially if the rabbit is stressed or the weather changes (affecting ear pressure).
The first milestone is the rabbit eating on its own. Once they can maintain their weight without syringe feeding, the pressure on the owner lightens. The second milestone is the cessation of rolling. Even if the tilt remains, a rabbit that can stand and move purposefully is a rabbit that is winning the battle.
| Phase | Duration | Focus of Care |
| Stabilization | Days 1–3 | Maintaining appetite & stopping the roll |
| Observation | Weeks 1–2 | Monitoring medication response & hydration |
| Compensation | Months 1–3 | Neurological adaptation to the “new normal” |
Managing Long-Term Effects
It is a misconception that a permanent tilt means a poor quality of life. Many rabbits retain a lean but are perfectly capable of binkying and grooming. When my own rabbits, Mocha and Chino, encountered minor balance issues, I learned that they don’t care about being “straight”—they only care about being comfortable.
The rabbit’s brain is remarkably plastic. Over time, they will learn to compensate for the bad balance data by relying more on their vision and whiskers. You may notice them “scanning” (moving their head back and forth) to get a better sense of depth. This is a sign of a high-functioning, adapted brain.
10. Quality of Life with Permanent Tilt
Yes. Rabbits often adapt through “vestibular compensation,” where the brain gradually learns to adjust to abnormal balance signals from the damaged ear or nervous system. They may need lower-entry litter boxes, padded flooring, and safer enclosure layouts, but many continue to live active, happy lives. Helpful guidance for caring for disabled or mobility-impaired rabbits is also available from House Rabbit Society
You should also pay attention to the “down” side of the face. The eye that is closest to the ground is prone to drying out or getting scratched. Regular use of lubricating eye drops and keeping the area clean of debris is a simple but vital part of long-term care. If they can still interact with their bonded partner and get excited for treats, their quality of life is high.
Unfortunately, yes. Chronic ear disease or a reactivation of E. cuniculi during times of stress can cause a relapse. Relapses often happen during season changes, after a move, or if the rabbit loses a bonded partner. Long-term monitoring and maintaining a low-stress environment are your best preventative measures.
Owners should keep a “emergency kit” on hand, including a fresh bag of Critical Care and a syringe. If you notice even a 5-degree increase in the tilt, restarting anti-inflammatories immediately (under vet guidance) can often nip a relapse in the bud before the rolling starts again.
12. Immediate Indicators for Veterinary Care

If you observe your rabbit:
- Rolling uncontrollably or thrashing
- Unable to stand or reach food/water
- Showing rapid, rhythmic eye movements (nystagmus)
- Producing significantly fewer or smaller droppings
Take them to a rabbit-savvy vet immediately. Early intervention is the primary difference between a full recovery and a permanent decline. Because rabbits are prey animals, they hide their pain; if you are seeing these signs, the rabbit has likely been struggling for longer than you realize.
13. Frequently Asked Questions
Can head tilt go away on its own?
No. It indicates a serious underlying issue like a parasitic or bacterial infection that will only worsen without medical intervention.
Is rabbit head tilt contagious?
E. cuniculi spores are shed in urine and can be contagious to other rabbits. Bonded partners should usually be treated alongside the symptomatic rabbit.
How long does recovery take?
Stabilization usually happens in days, but neurological healing can take weeks or months. Don’t give up in the first week!
Can a rabbit with a permanent tilt be happy?
Absolutely. As long as they can eat, move, and interact normally, many rabbits with a permanent head tilt can still enjoy a very high quality of life. You can find adaptive housing and care ideas from PDSA
14. Conclusion
Head tilt is terrifying to witness, but it isn’t an automatic death sentence. With aggressive treatment and supportive nursing care, many rabbits bounce back. Early intervention is the key; if you see a lean, act immediately. Your rabbit’s ability to adapt is their greatest strength, and with your help, they can navigate their tilted world with ease. One day at a time, your “wonky” bunny can return to a life of binkies and head rubs.
Medical & Veterinary Disclaimer: bunnyowners.com is an informational resource for rabbit owners and enthusiasts. We are not veterinarians. The content on this website is not a substitute for professional veterinary care, diagnosis, or treatment. Always seek the advice of your veterinarian with any questions you may have regarding your pet’s medical condition, diet, or overall health.
